Anti Cancer Medicine
Price 30000 INR/ Unit
Anti Cancer Medicine Specification
- Dosage Form
- As Per Suggestion
- Origin
- India
- Feature
- Other
- Ingredients
- Other
- Application
- Other
- Storage Instructions
- Cool & Dry Place
- Shelf Life
- 2 Years
Anti Cancer Medicine Trade Information
- Minimum Order Quantity
- 1 Box
- FOB Port
- Delhi, Mumbai
- Payment Terms
- Letter of Credit (L/C), Letter of Credit at Sight (Sight L/C), Paypal, Western Union, Telegraphic Transfer (T/T), Cash in Advance (CID), Cheque, Cash Advance (CA)
- Supply Ability
- 10000 Boxes Per Month
- Delivery Time
- 7 Days
- Packaging Details
- 1 Vial per box
- Main Export Market(s)
- Australia, North America, Eastern Europe, Western Europe, Africa, Central America, Middle East, South America, Asia
- Main Domestic Market
- All India
- Certifications
- US FDA, WHO GMP
About Anti Cancer Medicine
Anti-cancer drugs, sometimes referred to as chemotherapy drugs or anticancer drugs, are a broad category of treatments used to treat cancer. By interfering with cancer cells' DNA synthesis, cell division, or particular signalling pathways, these medications aim to target and prevent the growth and spread of cancer cells. They can be given by a variety of ways, including intravenous infusions, injections, and oral tablets. To achieve the best therapeutic results, anti-cancer medications are frequently combined with surgery, radiation therapy, or immunotherapy. The type of cancer, its stage, and the patient's condition all influence the medication choices and treatment plan. These drugs may have adverse effects, but they are carefully monitored by medical specialists to ensure the best possible patient care.
Features of Anti Cancer Medicines:
2. Different Drug Classes: There are numerous anti-cancer medications that fall under various classes, allowing for customised treatment plans based on the kind and stage of cancer.
3. Combination Therapies: To improve the efficacy of cancer treatments, these drugs may be used in conjunction with other cancer therapies such surgery, radiation therapy, or immunotherapy.
4. Route of delivery: To provide flexibility in therapy delivery, anti-cancer medications are available in a variety of formulations, including oral tablets, intravenous infusions, and injections.
5. Dosage Modification: Based on the answers of each patient, healthcare practitioners can modify the dosage of anti-cancer medications, reducing side effects while preserving therapeutic efficacy.
Anti Cancer Medicines Benefits:
1. The ability of anti-cancer medications to kill cancer cells or stop their proliferation, which results in tumour reduction or removal, is its main advantage.
2. Increased Survival Rates: The usage of these medications has helped increase survival rates for several cancer types.
3. Anti-cancer medications can provide palliative care for people with advanced cancer, reducing symptoms and enhancing quality of life.
4. Early-Stage Treatment: These drugs are used as adjuvant therapy in some malignancies to stop the spread of the disease following surgery.
5. Control of Metastatic Cancer: Anti-cancer medications can prevent the spread of cancer to other body parts (metastasis), hence extending patient life and enhancing disease management.
6. Neoadjuvant Therapy: These drugs are occasionally used as neoadjuvant therapy to reduce tumour size prior to surgery or radiation treatment.
7. Personalised Approach: Oncologists can modify treatment regimens based on the particular cancer kind, stage, and personal characteristics of the patient, assuring the best and most appropriate care.
8. Complimentary Medicine Synergy: Anti-cancer medications can produce synergistic effects when used with other cancer treatments, improving treatment outcomes.
9. Ability Cure: These medications have the ability to cause cancer remission in some patients, which presents the possibility of a cure.
10. Research & Innovation: Anti-cancer drug developments and ongoing research are broadening the range of available treatments and enhancing patient outcomes.
Anti-cancer medications can have major positive effects, but they may also have negative consequences that need to be carefully handled by medical professionals in order to improve patient care and treatment outcomes. The use of these medications necessitates competence, and patients and their oncologists should work together to decide on the best course of treatment while taking into account each patient's circumstances and treatment objectives.
Anti Cancer Medicines Applications:
1. Treatment for Cancer: Breast cancer, lung cancer, colon cancer, prostate cancer, leukaemia, lymphoma, and ovarian cancer are just a few of the many cancers that are treated using anti-cancer medications.
2. Adjuvant Therapy: These drugs are frequently used as adjuvant therapy following surgery or radiation to eliminate any cancer cells that may still be present and lower the chance of cancer recurrence.
3. Neoadjuvant Therapy: Before surgery or radiation, anti-cancer medications may be used in some circumstances to shrink tumours and make them more amenable to operation.
4. Palliative Care: In advanced cancer stages, anti-cancer medications are used to treat symptoms, slow the growth of tumours, and enhance patients' quality of life.
5. Targeted Therapy: Some anti-cancer drugs are made to target particular molecular abnormalities in cancer cells, resulting in a more individualised and efficient course of treatment.
6. Combination Therapy: To improve treatment outcomes, they are used in conjunction with other cancer treatments including radiation therapy or immunotherapy.
What are the Side Effects of Anti Cancer Medicines:
1. Anti-cancer medications have the potential to suppress bone marrow, which can result in anaemia, a higher risk of infections, and bleeding issues.
2. Numerous anti-cancer medications might result in nausea and vomiting.
3. Hair Loss: Alopecia, or temporary hair loss, is a side effect of some drugs.
4. Patients may feel weak or worn out while receiving treatment.
5. Constipation or Diarrhoea: Digestive issues like constipation or diarrhoea could happen.
6. Skin Reactions: Some people may encounter skin issues like rashes or photosensitivity.
7. The Hand-Foot Syndrome is a skin reaction that manifests as redness, swelling, and peeling of the palms and soles and is brought on by some medications.
8. Some anti-cancer medications have the potential to cause neurological side effects, such as peripheral neuropathy.
9. Infertility: In some situations, these medications might lead to infertility that is either temporary or permanent.
10. Cardiac Toxicity: Some anti-cancer medications may have an impact on the circulatory system and the heart.
11. Liver and Kidney Toxicity: Some medications can harm the liver or the kidneys.
12. Anti-cancer medications have been shown to decrease the immune system, increasing the risk of infections in patients.
Healthcare professionals should regularly monitor patients taking anti-cancer medications to manage any adverse effects and guarantee treatment safety. To get the best results while minimising side effects, using these medications requires knowledge and personalised treatment strategies. To enhance the overall experience of cancer treatment, healthcare professionals collaborate closely with patients to optimise treatment schedules and offer supportive care.
Advanced Cancer Treatment
This medicine harnesses Trastuzumab, a well-established anti-cancer agent, offering hope to patients diagnosed with breast cancer and leukemia. Its targeted action supports effective therapy as part of broader cancer management strategies.
Proper Storage for Potency
To maintain the effectiveness of the medicine, strict storage conditions are essential. It should be stored at 2C to 8C in a cool, dry location, away from excessive heat or humidity, to preserve its stability and potency throughout its shelf life.
FAQ's of Anti Cancer Medicine:
Q: How should the anti-cancer medicine containing Trastuzumab 440mg be stored?
A: This medication must be stored in a refrigerator at temperatures between 2C to 8C and kept in a cool, dry place. Proper storage is critical to preserve its quality and therapeutic effectiveness.Q: What is the recommended usage for this anti-cancer medicine?
A: The medicine is intended for the treatment of breast cancer and leukemia. The exact dosage and administration guidelines should be strictly followed as prescribed by a qualified physician.Q: When should this medicine be administered?
A: Administration timing and frequency are determined by a healthcare provider, based on the patient's clinical condition and response to treatment. Always adhere to your physician's instructions regarding dose and schedule.Q: Where is this anti-cancer medicine manufactured and supplied from?
A: This product is manufactured, distributed, exported, and supplied by certified entities in India. It is accessible both domestically and internationally through authorized suppliers.Q: What is the physical form and shelf life of this drug?
A: The medicine is supplied in liquid form and has a shelf life of two years when stored properly according to the specified temperature conditions.Q: How does Trastuzumab 440mg benefit cancer patients?
A: Trastuzumab targets specific cancer cells, particularly in breast cancer and leukemia, helping to slow disease progression and improve treatment outcomes as part of a comprehensive cancer therapy plan.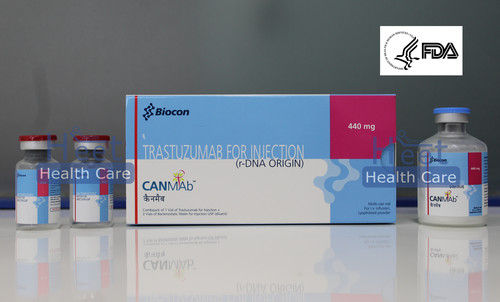

Price:
- 50
- 100
- 200
- 250
- 500
- 1000+
More Products in Anti Cancer Medicine Category
Alkacel Melphalan 2mg Tablet
Price 1000 INR / Piece
Minimum Order Quantity : 10 Pieces
Feature : Other
Application : Other
Storage Instructions : Cool & Dry Place
Dosage Form : As Per Suggestion
Veenat Imatinib 400 mg Tablets
Price 2500 INR / Box
Minimum Order Quantity : 10 Boxes
Feature : Other
Application : Other
Storage Instructions : Store Imatinib Tablets in a cool, dry place, away from direct heat and light.
Dosage Form : As Per Suggestion
Erlocip Erlotinib Tablets IP 150 mg
Price 5000 INR / Box
Minimum Order Quantity : 10 Boxes
Feature : Other
Application : Other
Storage Instructions : Cool & Dry Place
Dosage Form : As Per Suggestion
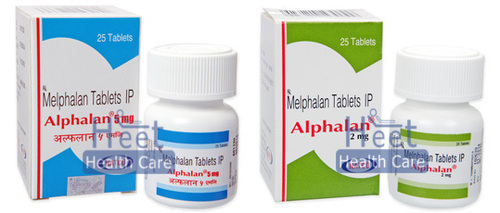
Alphalan Melphalan 2mg Melphalan 5mg Tablets
Price 5000 INR / Box
Minimum Order Quantity : 100 Boxes
Feature : Other
Application : Other
Storage Instructions : Cool & Dry Place
Dosage Form : As Per Suggestion

 Send Inquiry
Send Inquiry Send Inquiry
Send Inquiry
 English
English Spanish
Spanish French
French German
German Italian
Italian Chinese (Simplified)
Chinese (Simplified) Japanese
Japanese Korean
Korean Arabic
Arabic Portuguese
Portuguese